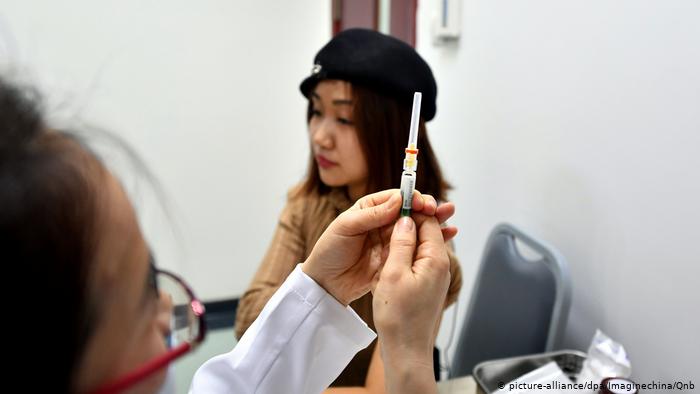
Vaccines against human papillomavirus (HPV) could wipe out cervical cancer within decades in wealthy nations, scientists say, after a major study showed a stark reduction in cancer-causing infections.
Rates of genital and anal warts, precancerous lesions and infections have dramatically declined among young people since the implementation of HPV vaccination programs in high-income countries like Germany, the UK and Australia.
Read more: Anti-vaxxer mentality is better tackled through empathy, not facts
“This is a really good example of the population impact of vaccination and what herd immunity can do,” Thomas Harder, from the Immunization Unit at the Robert Koch Institute in Berlin, told DW.
Success in high-income countries
Human papillomavirus is sexually transmitted and the major cause of cervical cancer. More than 500,000 women are diagnosed with cervical cancer each year and over 300,000 die from it, according to the World Health Organization.
Read more: Richer countries show lower trust in vaccines
The research, published in The Lancet, analyzed the health outcomes of 66 million people under 30 in 14 high-income countries, including Germany. It showed that, in countries where the vaccine had been given out for more than five years, there was an 83% reduction in two strains of HPV in 15 to 19 year-old girls and a 66% reduction in women aged 20 to 24.
Boys and men were also shown to have benefitted; anal and genital warts reduced by half among teenage boys and by a third for those between 20 to 24. Warts also dropped by 67% among teenage girls, 54% among women aged 20 to 24 and 31% in women aged 25 to 29.
Read more: Measles hot spot pediatrician’s office?
As the HPV vaccine has only been available for around 10 years, it’s too soon to measure how these programmes might impact rates of cervical cancer itself, but scientists say the results so far are promising.
Need in low-income countries
“Nearly 100% of cervical cancers are caused by HPV,” Harder said. “If we’re able to eliminate HPV by vaccination, we’re able to eliminate cervical cancer.”
Many more women die of cervical cancer in low-income countries, which weren’t represented in the study. It’s these places that Harder says could benefit most from HPV vaccination programs, as regular cervical screening and treatment is often expensive and difficult to carry out.
“For many of these countries, [vaccinating] high numbers of girls might actually be the easier way, as it’s not easy to regularly screen women and monitor them,” explained Harder.
Not just cervical cancer
The HPV vaccine is also expected to reduce the rates of other HPV-induced cancers in the future, Harder points out, like anal, penile, mouth and throat cancer.
“With the vaccination, we will hopefully see a decline in these more rare forms of cancer,” he said.
As for other vaccinations that target cancer-causing infections, Harder highlights Hepatitis B-induced liver cancer. This form of cancer has been effectively reduced in some parts of Southeast Asia thanks to Hepatitis-B vaccination programs.
“When the vaccination was introduced, we saw a sharp decline in cases of liver cancer within just a few years,” he said.
In Germany, the HPV vaccination program has been in place for preteen girls for the last 10 years, and as of last year, boys aged 12 to 13 are now also given the vaccination. While Harder says there isn’t current nationwide data on the health outcomes of people vaccinated against HPV in Germany to the same degree as other countries, so far there is evidence the vaccine has had strong effects on HPV infections, precancerous lesions and genital warts.
Despite the success rate of global immunization programs like the HPV vaccine — which has been given to more than 270 million people worldwide — anti-vaxx groups still spread misinformation about the vaccine, including that it causes paralysis and sudden death in young women and increases their sexual libido.
It’s been so effective worldwide, though, that the Center for Disease Control in the US recently agreed on the recommendation that women up to the age of 45 consult with their doctors about getting the vaccine.
Although usually it’s considered ineffective for people who are already sexually active and have been exposed to the virus, it can still offer protection for people who, for example, have had none or very few sexual partners and plan to start dating again.