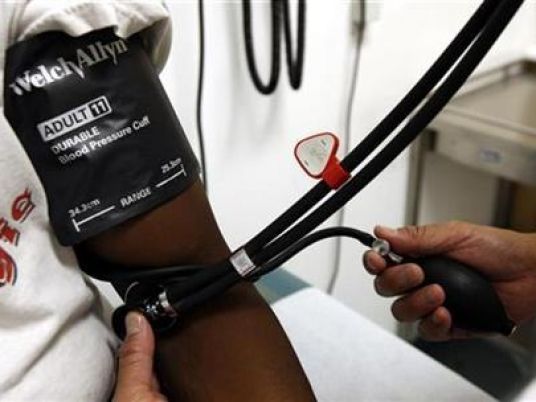
Racial minorities may be more likely to forego colon cancer screening than whites because their healthcare providers don’t recommend the potentially life-saving tests, a new study in California suggests.
“It was interesting because this study suggests that one of the things we need to do . . . is talk to doctors,” said Dr. Folasade May, who led the study.
“We can do all the public policy we want, but we need to make it very clear to providers that they should emphasize colon cancer screening and more importantly recommend colon cancer screening to patients of all ethnic backgrounds,” May said.
Colon cancer is the second leading cause of death in the US. The Centers for Disease Control and Prevention estimates that 49% of African Americans, 37% of Latinos and 48% of Asian Americans over age 50 were screened in 2008, compared to 56% of whites.
African Americans have the highest incidence of colon cancer and death from that disease of any race in the US, the study authors point out in a paper online now in the American Journal of Gastroenterology. Latinos have the highest rate of advanced colon cancer and are less likely to survive than whites. Colon cancer is the third leading cause of death for Asian Americans.
“Even though colon cancer screening uptake is poor overall in the US, uptake is especially poor in underserved groups,” said May, a gastroenterologist at the Cedars-Sinai Center for Outcomes Research and Education in Los Angeles.
Past studies have shown that health care provider recommendations can help persuade patients to be screened. So May, who joins the faculty of the David Geffen School of Medicine in July, and his colleagues decided to look at whether lack of a doctor’s recommendation contributes to lagging screening rates in minority communities.
The researchers analyzed responses to the 2009 California Health Interview Survey, which asked participants about their health, visits to healthcare providers and health insurance.
The 5,793 people in the analysis were 50 to 75 years old. None had been screened for colon cancer by any of the accepted tests, including sigmoidoscopy, colonoscopy or fecal occult blood test. Just over half of the group was white, 21% Latino, 12% Asian, 5.3% African American and the rest “other.”
When asked “the main reason” they had not had colon cancer screening, participants were given a choice of several possible answers. About 19% selected “Doctor did not tell me I needed the test.” A little over 20% chose “no reason/did not think about it.” Smaller percentages of the group chose other responses that blamed a lack of insurance coverage, procrastination or laziness, not having any symptoms, or fear of unpleasantness of the tests themselves.
Only 17% of whites said their primary reason for skipping screening was a lack of doctor recommendation, compared to 25% of African Americans, 21% of Latinos and 22% of Asian Americans.
After adjusting for race, age, sex, education, health and other factors, African Americans were 46% more likely than whites to report non-recommendation as their main reason for not getting screened.
Non-English speaking Asian Americans were much less likely to cite non-recommendation as the primary reason for not getting screened than non-English speaking Whites or English-speaking Asian Americans.
May said providers might not recommend screening to racial minorities because of their other chronic health problems or because the doctors thought the patients would be fearful of the tests.
“A provider tasked with the responsibility of addressing many important medical concerns during a patient visit may just not have the time to also discuss colon cancer screening or breast cancer screening,” May told Reuters Health.
Dr. Kevin Schulman of the Duke University School of Medicine in Durham, North Carolina, said the healthcare system could be the problem, rather than individual doctors.
“It just may be that they lack access, they may not have a routine source of care, they may have issues with health insurance,” Schulman said. “But those are all just symptoms of the complexity of the system.”
Schulman, who studies health policy and economics, said if patients consistently saw one doctor over time, “vulnerable people would have much less of a challenge getting access.” Getting the word out to everyone would help, he said.
When May asked African American participants for suggestions to improve screening rates, they told her the media should publicize the importance of screening and influential celebrities should recommend it.
“Some African Americans said, ‘Why don’t you get someone like Denzel Washington or President Obama to have a colonoscopy on TV,’” May noted.



